Swedish researchers have made a significant breakthrough in the field of medical technology by developing a microscale device for implantation in the eye. This device offers exciting possibilities for cell-based treatments of disorders like diabetes. The team responsible for this innovation hails from the KTH Royal Institute of Technology and Karolinska Institutet and has published their findings in the journal Advanced Materials.
The 3D-printed device is designed to encapsulate insulin-producing pancreatic cells along with electronic sensors. It’s a unique tool that can be precisely positioned within the eye without the need for sutures. This development has the potential to revolutionize cell-based therapies, particularly for treating both Type 1 and Type 2 diabetes, with the eye serving as a suitable location for these treatments.
“The eye is our only window into the body, and it’s immune-privileged,” Herland states.
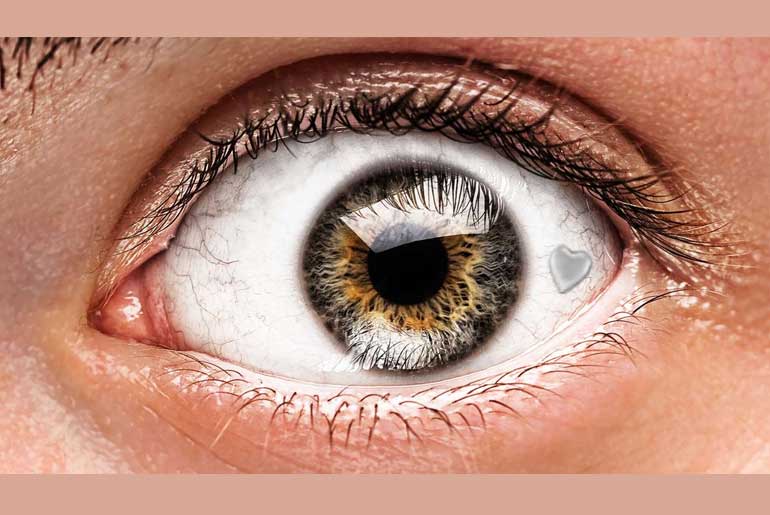
Anna Herland, a senior lecturer involved in the research, highlights the eye’s suitability for this technology due to its lack of immune cells that typically react negatively during the initial stages of implantation. The eye’s transparency also allows for easy visual and microscopic monitoring of the implanted device’s behavior over time. The device itself is shaped like a wedge, approximately 240 micrometers in length, enabling mechanical fixation between the iris and the cornea in the anterior chamber of the eye (ACE).
“We designed the medical device to hold living mini organs in a micro-cage and introduced the use of a flap door technique to avoid the need for additional fixation,” states Wouter van der Wijngaart, professor in the Division of Micro- and Nanosystems at KTH.
One remarkable achievement of this work is the successful mechanical fixation of a device in the anterior chamber of the eye, as demonstrated in tests on mice. The implanted device remained in place within the living organism for several months, and the mini organs it contained quickly integrated with the host animal’s blood vessels, functioning normally. Per-Olof Berggren, a professor of experimental endocrinology at Karolinska Institutet, contributed his extensive experience in transplanting islets of Langerhans to the anterior chamber of the eye in mice.
“The current unit is unique and will among other things form the basis for our continued work to develop an integrated microsystem for studying the function and survival of the islets of Langerhans in the anterior chamber of the eye,” Berggren states. “This is also of great translational importance, as transplantation of Langerhans islands to the anterior chamber of the eye in humans is subject to clinical trials in patients with diabetes.”
“Ours is a first step towards advanced medical microdevices that can both localize and monitor the function of cell grafts,” she states.
This breakthrough overcomes a significant obstacle in the development of cell therapies, particularly for diabetes. The design of the device eliminates the need for invasive monitoring methods to assess the graft’s function and guide care to ensure long-term transplant success. Additionally, the design ensures that mini organs such as organoids and islets of Langerhans receive the necessary supply of nutrients without any restrictions. This promising development opens up new horizons in the field of medical treatments and the potential for more effective, less invasive therapies for various disorders.
Disclaimer:
The information contained in this article is for educational and informational purposes only and is not intended as a health advice. We would ask you to consult a qualified professional or medical expert to gain additional knowledge before you choose to consume any product or perform any exercise.