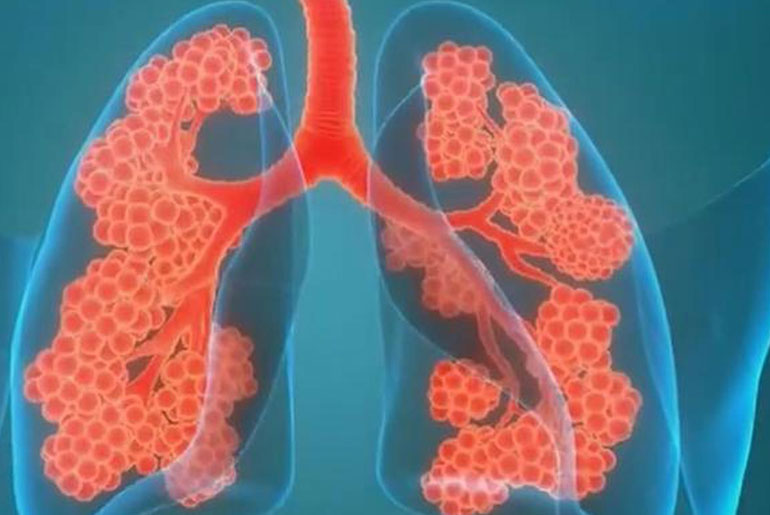
The findings of the study conducted by Christian Medical College, Vellore, shed light on the significant impact of COVID-19 on the respiratory health of Indian survivors. Published in the PLOS Global Public Health journal, the research focused on assessing the effects of COVID-19 on lung damage and quality of life among Indians during the first wave of the pandemic. The study, involving 207 participants, revealed that Indian COVID-19 survivors experienced more substantial lung function impairment compared to their European and Chinese counterparts, as observed in other published cohorts primarily comprising Caucasian subjects.
The research employed various assessments, including lung function testing, exercise tolerance evaluations, chest radiography, and measurements of quality of life, to study the post-COVID-19 lung damage in recovered patients. These findings underscore the need for targeted strategies and interventions to address and improve respiratory health outcomes in individuals recovering from COVID-19, especially in the Indian population.
The study highlights the potential long-term consequences of COVID-19 on lung health, indicating that while many individuals may recover within a year of the infection, some could experience permanent lung damage for life. The research conducted by Christian Medical College, Vellore, involved a comprehensive assessment of lung function and quality of life among COVID-19 survivors. The subjects underwent various evaluations, including pulmonary function tests, six-minute walking tests, chest radiography, and completion of the St. George’s respiratory questionnaire.
“In a large Indian cohort, we have reported the presence of post-Covid-19 residual lung damage, as assessed by lung function tests, exercise capacity, chest radiography and quality of life measurements. Our population reported relatively higher symptomatology and comorbidities and greater lung function impairment, compared to most published studies. We have shown that post-Covid-19 lung damage results in significant impairment of lung function, quality of life and effort tolerance,” stated the study.
The signs and symptoms of post-COVID lung damage:
The signs and symptoms of post-COVID lung damage, also known as post-acute sequelae of SARS-CoV-2 infection (PASC) or long COVID, can vary among individuals. Here are some common manifestations that may indicate lung damage:
- Shortness of breath: Difficulty in breathing, especially during physical activity, may persist long after the acute phase of the infection has passed.
- Persistent cough: A lingering cough that lasts for weeks or months after the initial infection is a common symptom of post-COVID lung damage.
- Chest pain or tightness: Some individuals may experience chest pain or tightness, which can be exacerbated by deep breathing or exertion.
- Fatigue: Chronic fatigue is a prevalent symptom, often accompanied by reduced exercise tolerance.
- Decreased exercise tolerance: Individuals may notice a reduced ability to engage in physical activities they once tolerated, likely due to persistent shortness of breath or fatigue.
- Frequent respiratory infections: Lung damage from COVID-19 can weaken the immune system, increasing vulnerability to respiratory infections.
It’s important to note that the severity and duration of these symptoms can vary from person to person. Individuals experiencing persistent symptoms after recovering from COVID-19 should seek medical attention. Healthcare professionals can conduct thorough evaluations, which may include lung function tests, imaging studies, and other diagnostic procedures, to assess the extent of lung damage and determine an appropriate course of action for management and rehabilitation.
Managing post-COVID lung damage:
Managing post-COVID lung damage requires a comprehensive and multidisciplinary approach. Here are some treatment strategies that may be employed:
- Pulmonary Rehabilitation: Structured exercise programs supervised by healthcare professionals can aid in improving lung function, increasing endurance, and enhancing overall physical health. These programs may include breathing exercises, aerobic conditioning, and strength training.
- Medications: Depending on the specific symptoms and conditions, healthcare providers may prescribe medications such as bronchodilators or anti-inflammatory drugs to alleviate symptoms like shortness of breath and inflammation in the airways.
- Oxygen Therapy: In cases of severe lung damage where oxygen levels are compromised, supplemental oxygen therapy may be necessary. This helps ensure that the body receives an adequate supply of oxygen.
- Nutritional Support: A balanced and nutritious diet is crucial for overall health and recovery. Adequate hydration and proper nutrition can support the body in its healing process.
- Psychological Support: Dealing with chronic symptoms can impact mental health. Counseling, therapy, or support groups may be beneficial in helping individuals cope with the emotional and psychological aspects of post-COVID lung damage.
- Regular Monitoring: Close monitoring by healthcare providers is essential to track the progress of the individual, adjust treatment plans as needed, and address any emerging complications. Regular follow-ups allow for a proactive approach to managing post-COVID lung damage.
It’s important for individuals experiencing post-COVID lung damage to work closely with their healthcare team, which may include pulmonologists, physical therapists, nutritionists, and mental health professionals, to develop a personalized treatment plan based on their specific needs and symptoms.
Disclaimer:
The information contained in this article is for educational and informational purposes only and is not intended as a health advice. We would ask you to consult a qualified professional or medical expert to gain additional knowledge before you choose to consume any product or perform any exercise.