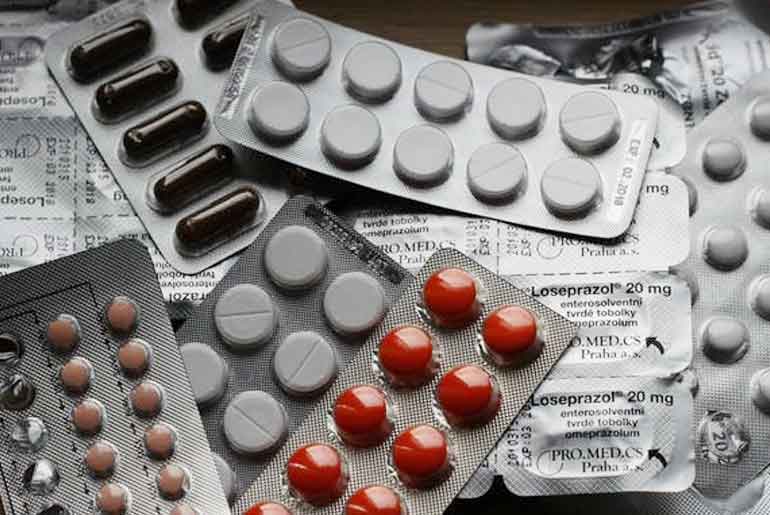
A recent study has uncovered that medications used to manage various chronic diseases may impede the body’s ability to regulate its core temperature effectively, leading to potential challenges in heat dissipation and thermoregulation. This situation holds significant implications for elderly individuals undergoing treatment for conditions like cancer, cardiovascular issues, Parkinson’s disease, dementia, and diabetes, especially in hot weather.
The research delved into investigating the connections and impacts of medications on thermoregulation. The study’s results were presented in a comprehensive manner, focusing on medication classes commonly prescribed for prevalent chronic conditions such as cardiovascular disease, neurodegenerative disease, diabetes, and cancer. Published in Pharmacological Reviews under the title “Effects of Medications on Heat Loss Capacity in Chronic Disease Patients: Health Implications Amidst Global Warming,” the findings unveiled those medications used for common chronic conditions—like blood thinners, blood pressure drugs, medications for Parkinson’s disease and Alzheimer’s disease, and select chemotherapy drugs—can exacerbate the challenges the human body faces in managing hot weather. This interference can manifest as reduced sweating or diminished blood flow to the skin.
Lead author and second-year PhD candidate from the Human Potential Translational Research Programme Jericho Wee stated, “Rising global temperatures caused by climate change pose a significant health concern for clinical patients reliant on long-term medications and healthcare. Increasingly, we will continue to see more elderly patients, many who have multiple health conditions and are taking different types of medication concurrently to manage their chronic diseases, compounding the risk of heat-related illness and dehydration. Understanding how each medication impacts thermoregulation, in the face of warmer environments, is the crucial first step to predicting the possible health outcomes when multiple medications are taken concurrently.”
While previous reviews have explored the connection between medications and heat, this study provided a broader context by examining these effects in relation to chronic diseases and the aging process. Notably, patients receiving certain cancer medications reported experiencing symptoms like hot flushes, including inappropriate sweat responses and elevated core temperatures, impacting their quality of life.
Senior author Assoc Prof Jason Lee stated, “This review emphasises the importance of studying the mechanisms of altered thermoregulation in individuals with diabetes and other cardiometabolic conditions to prevent heat-induced conditions. This is most relevant in Singapore and many other countries, where we have rapidly ageing populations and rising ambient temperatures. Pharmacological and thermal physiologists should focus transdisciplinary efforts on this area of research to refine and enhance safe medication prescription guidelines to preserve the health of people who need these medications, even in hot weather.”
Assoc Prof Melvin Leow, the review’s co-author and Senior Consultant Endocrinologist at Tan Tock Seng Hospital stated, “Physicians are often unaware of the potential harms certain drugs may cause by compromising the body’s thermoregulatory control mechanisms. This is an especially important area to delve into as those with chronic diseases and older adults are susceptible to adverse health outcomes in the heat, due to their reduced thermoregulatory capacity. It is timely and prudent that scientists and doctors collaborate even closer in this important field that cuts across a wide range of medical disciplines.” The study was supported by the National Research Foundation, Prime Minister’s Office, Singapore under its Campus for Research Excellence and Technological Enterprise (CREATE) Programme.
The study emphasized the role of exercise and improved fitness levels in mitigating the frequency of hot flushes and enhancing thermoregulatory responses, even in other chronic conditions like diabetes. However, chemotherapy and medications may limit patients’ ability to exercise, leading to a cycle of decreased exercise capacity critical for their recovery.
The research highlighted specific implications for various chronic diseases:
- Cardiovascular Disease: Patients with cardiovascular diseases, such as heart disease and stroke, face increased vulnerability to heat exposure due to the strain on their hearts. Certain medications like anti-platelet medications and beta-blockers can further impact thermoregulation, potentially leading to heat stroke.
- Diabetes: Insulin, used to manage high blood sugar, can impair heat regulation and increase metabolic heat production, which could be harmful in situations where heat dissipation is compromised. Metformin, a medication for Type 2 diabetes, can lead to dehydration, amplifying cardiovascular strain during heat stress.
- Neurocognitive Diseases: Patients with Parkinson’s and Alzheimer’s disease experience thermoregulatory dysfunction due to altered dopamine and acetylcholine levels. Medications for these conditions can affect the brain’s control of thermoregulation, potentially leading to hyperthermia or hypothermia.
The study underscores the necessity for medical practitioners to be aware of these potential side effects and for closer collaboration between scientists and doctors to address these complexities, given their far-reaching impact. As global temperatures continue to rise due to climate change, the findings emphasize the need for careful consideration of medication effects on thermoregulation, especially in vulnerable populations.
Disclaimer:
The information contained in this article is for educational and informational purposes only and is not intended as a health advice. We would ask you to consult a qualified professional or medical expert to gain additional knowledge before you choose to consume any product or perform any exercise.