A recent meta-analysis titled “A meta-analysis of previous falls and subsequent fracture risk in cohort studies” found a notable correlation between self-reported falls and heightened fracture risk. Interestingly, the study also revealed that men tend to have a slightly higher risk of fractures compared to women, despite both genders reporting increased fall occurrences. These findings underscore the importance of fall prevention strategies, particularly among older adults, to mitigate the risk of fractures and associated health complications.
The meta-analysis, published in Osteoporosis International, drew upon data from 46 prospective cohorts involving over 900,000 individuals. It highlighted the significance of incorporating previous falls into patients’ medical histories, particularly when utilizing fracture risk assessment tools like the FRAX (Fracture Risk Assessment) Tool. By including information about prior falls, clinicians can more accurately assess an individual’s risk of experiencing fractures over the next decade.
Given that FRAX is one of the most widely utilized tools for predicting fracture risk, this recommendation underscores the importance of enhancing its predictive accuracy by accounting for previous falls. This integration can contribute to more informed clinical decision-making and targeted interventions aimed at reducing the burden of fractures, especially among high-risk populations.
The FRAX tool, developed using longitudinal data from global studies, has historically not incorporated previous falls into its algorithm. However, a recent update to the FRAX dataset included previous falls as a significant risk factor, revealing that they indeed elevate the risk of fractures. This inclusion highlights the importance of falls as a contributor to fracture risk in both men and women, with men experiencing a slightly higher risk. These findings emphasize the necessity of considering previous falls in fracture risk assessment tools like FRAX to enhance their accuracy and provide more comprehensive risk evaluation for patients, aiding in the prevention and management of fractures.
Key Findings of the Meta-Analysis:
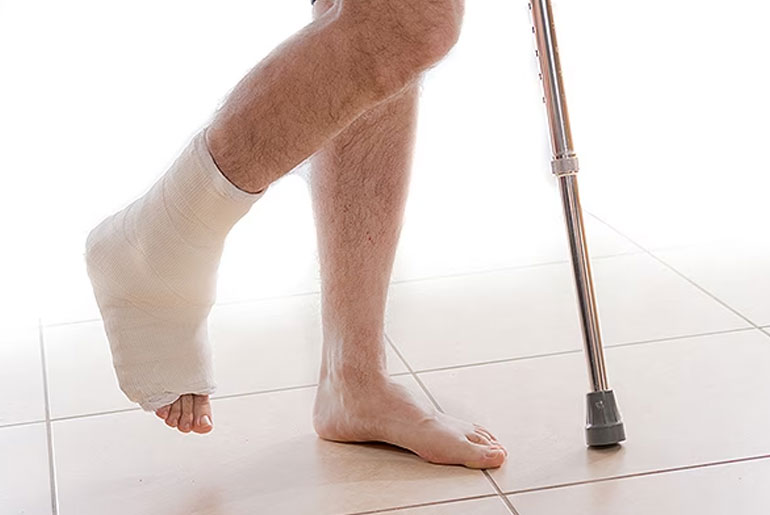
- Increased Fracture Risk: Individuals with a history of falls within the past year were found to have a significantly higher risk of various types of fractures, including any clinical fracture, osteoporotic fracture, major osteoporotic fracture, and hip fracture. This indicates that a history of falls is strongly associated with an increased risk of experiencing fractures.
- Risk of Death: One or more previous falls were significantly associated with an increased risk of death among both women and men. This highlights the serious implications of falls beyond fracture risk, emphasizing the need for preventive measures to reduce fall-related morbidity and mortality.
- Sex Disparities: The association between previous falls and fracture risk varied by sex, with men exhibiting higher predictive values compared to women. This suggests that the impact of falls on fracture risk may differ between genders and underscores the importance of considering sex-specific factors in fracture prevention strategies.
- Independent Risk Factor: The increased fracture risk linked to previous falls was largely independent of bone mineral density, indicating that falls represent a standalone risk factor for fractures. This underscores the importance of assessing fall history alongside traditional risk factors like bone density when evaluating fracture risk.
- Clinical Implications: Integrating information about previous falls into fracture risk assessment tools like FRAX can enhance their predictive accuracy. This can help healthcare providers more accurately identify individuals at high risk of fractures and tailor preventive strategies accordingly. By improving risk prediction, healthcare providers can better guide interventions to reduce the incidence of fractures and improve patient outcomes.
In summary, the meta-analysis highlights the significant impact of previous falls on fracture risk, emphasizing the need for comprehensive assessment and preventive strategies to mitigate fall-related morbidity and mortality. Integrating fall history into fracture risk assessment tools can enhance their utility in clinical practice and aid in personalized fracture prevention strategies.
Disclaimer:
The information contained in this article is for educational and informational purposes only and is not intended as a health advice. We would ask you to consult a qualified professional or medical expert to gain additional knowledge before you choose to consume any product or perform any exercise.